Read an opinion piece examining how the public treated former Maricopa County Attorney Allister Adel’s battle with mental illness and alcohol use. Read more here.
mental illness
Patient Deaths at Arizona State Hospital Raise Questions About Staffing Levels, Lack of Oversight
NCDJ Board Member Becky Curran Kekula Discusses Facing the Fear of Inclusivity

By “The Morning Blend” show on TMJ-4 Milwaukee
NCDJ board member Becky Curran Kekula appeared on this morning talk show to discuss tips for treating people with disabilities fairly and respectfully. Part of the discussion focused on the fact that since 70% of disabilities are invisible, many people are nervous to either admit they have a disability, or to speak about someone who may have a disability that isn’t immediately apparent.
Also featured are some of Becky’s favorite tips for working remotely — a particularly relevant topic in the midst of the coronavirus pandemic.
Watch the full segment here: https://www.tmj4.com/shows/the-morning-blend/facing-the-fear-of-inclusivity
How to Accurately and Inclusively Cover Mass Shootings

In response to the recent mass shooting in El Paso, Texas, the National Association of Hispanic Journalists (NAHJ) has released a guide to help journalists “accurately and inclusively cover mass shootings.”
A full section of the NAHJ guide is dedicated to helping journalists cover gun violence without stigmatizing mental illness, or implying that a shooter’s mental illness caused or contributed to the violence. Among other recommendations, the NAHJ guide tells journalists that it is “inexcusable to mention the mental health issues the alleged killer might have been dealing with in an attempt to dismantle the reasoning behind this crime against humanity.” Additionally, the guide acknowledges that traumatic stories like the shooting in El Paso can be painful to cover and reminds reporters that it is always okay to reach out for help.
Click here to access How to Accurately and Inclusively Cover Mass Shootings on the NAHJ website.
Mother asks Maricopa County prosecutors to release her daughter, a 19-year-old with mental illness, from Lower Buckeye Jail
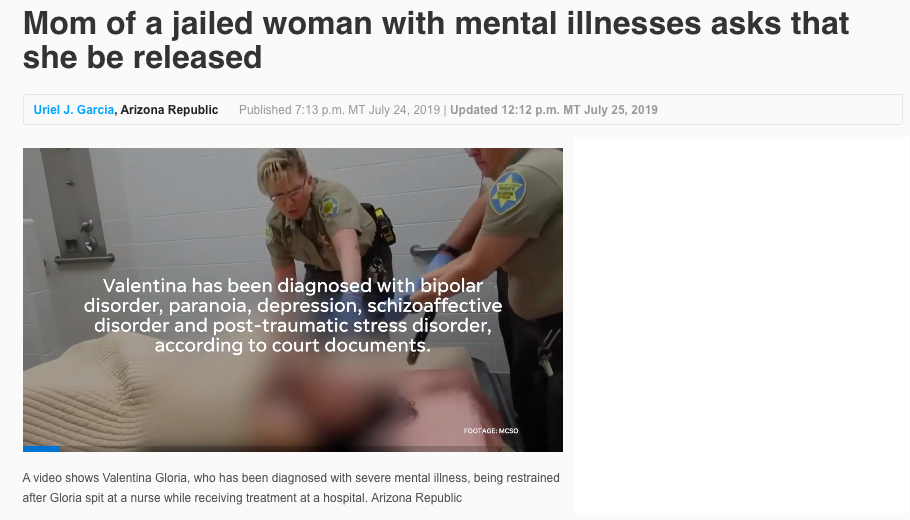
Valentina Gloria, a 19-year-old woman who has been diagnosed with several mental illnesses, has been detained at Maricopa County’s Lower Buckeye Jail for nearly six months, since February of this year. Now Vangelina Gloria, Valentina’s mother, is pleading for her teen daughter’s release.
Some say Valentina’s case exemplifies how our legal system criminalizes mental illness. Her predicament also highlights the ways in which our criminal justice system fails at providing quality mental healthcare to those who need it.
With support from Puente Arizona, a Phoenix-based migrant justice organization, Vangelina wrote a letter to Maricopa County Attorney Bill Montgomery earlier this week, requesting that he drop the charges against Valentina and release her from police custody. According to azcentral.com and court documents, Valentina has been diagnosed with bipolar disorder, paranoia, depression, schizoaffective disorder and post-traumatic stress disorder. Vangelina believes that being in jail is exacerbating her daughter’s mental health condition.
How did Valentina end up in jail?
In December 2018, [Valentina] Gloria was being treated in a behavioral health unit at St. Luke’s Hospital, where she was accused and arrested for spitting and punching two different nurses; she was then charged with two counts of aggravated assault. Then in May, a county judge ruled Valentina was incompetent to face the charges in court and ordered her to stay in jail to receive treatment through the County’s Restoration to Competency Program. A previous Arizona Republic analysis of Maricopa County’s Restoration to Competency Program expressed concerns about the program’s inefficiency and questioned the quality of the jailhouse mental healthcare provided by the county.
Click here to read an azcentral.com article recounting Vangelina’s efforts to secure Valentina’s release.
UPenn will offer new course on writing about mental health

Author, investigative journalist and Columbia J-school professor Stephen Fried will teach a new nonfiction writing course at University of Pennsylvania next semester. The course, which which will focus on writing about mental health and addiction, will be among the first undergraduate courses of its kind in the U.S.
Students taking the spring class, titled “Advanced Nonfiction Writing: Writing about Mental Health and Addiction,” will hear from guest lecturers and will read and discuss writings about behavioral health.
After covering mental health as a journalist for years, Fried said he understands the importance of teaching students how to report on these topics in a nuanced way. Uninformed writing about this subject matter can perpetuate the stigma surrounding mental illness and seeking psychiatric help.
Fried is the author of numerous books about the prescription drug industry and mental illness. In 2015 he co-authored Patrick Kennedy’s memoir A Personal Journey Through the Past and Future of Mental Illness and Addiction.
Read more about Fried’s new class at UPenn here.
Mishandling mental health crises to blame for spike in officer-involved shootings

What accounts for the sharp increase in the number of officer-involved shootings in Phoenix last year? A lack of mental health resources, according to a report released by the National Police Foundation on Friday. The report, which was commissioned by the city of Phoenix as a response to last year’s spike in incidences of officer-involved shootings, points to a number of underlying causes for the uptick. That police officers are fielding a growing number of 911 calls involving people with mental health issues is one of them.
Phoenix police officers who were interviewed for the study said they felt unprepared to respond to these kind of situations. Phoenix Police Chief Jeri Williams added that law enforcement officers shouldn’t be the first (or only) line of help available to people who are experiencing a mental health crisis and that many of the calls her department receives could be rerouted to alternative resources.
Read the Cronkite News story online. You can also download a copy of the National Police Foundation’s 72-page report here.
Class-Action Lawsuit Claims Stanford University Forces Suicidal Students to Leave School
According to an article published in the New York Times on August 28, the lawsuit accuses Stanford of “discriminating against students with mental health issues by coercing them into taking leaves of absences.” The lawsuit is the latest in a series of legal cases challenging mental health leave policies at schools like Princeton, George Washington University, Quinnipiac, and Hunter College. Read the New York Times story by Anemona Hartocollis here.

May articles highlight “Mental Health Month”
May is Mental Health Month and numerous organizations and celebrities are speaking up to raise awareness about the often taboo topic.
In a report for Cronkite News journalist Luke Wright focuses on famous athletes who describe their experiences with depression, panic attacks and suicide. The report features athletes from sports including basketball, football and track. The statistics mentioned in the story may shock from readers, for example Wright reports that, “Nearly 24 percent of 465 athletes at NCAA Division I private universities reported a “clinically relevant” level of depression, according to a 2016 study by researchers at Drexel and Kean universities. Female athletes had a higher prevalence rate: 28 percent vs. 18 percent.”
The science magazine “Nature” also features a collection of articles this month focused on mental health awareness in the science research industry. One article by Emily Sohn reports that graduate students are especially vulnerable to mental illness and includes tips from mental health experts on how to avoid it. In an opinion essay for “Nature” scientist Dave Reay describes his symptoms of depression as a “black dog,” similar to the one Winston Churchill made famous, that haunted his pursuit of a Ph.D.
In a story for NBC’s “Today Show” reporter Cynthia McFadden interviewed three teenagers with mental health disorders reacting positively to the social media campaign #MyYoungerSelf. The campaign features candid testimonies from sports and entertainment celebrities describing their experiences living with depression and anxiety.
Dancer says symptoms of OCD recede while he performs onstage
Steven Loch doesn’t know why his obsessive-compulsive disorder subsides while he’s dancing, but he’s grateful for the relief it provides from the “torture” of his symptoms. In a compelling interview with Brendan Kiley of The Seattle Times, Loch gives a candid description of the disturbing thoughts that cause his unpleasant behavior and prompted him to find treatment at psychiatric hospitals.
Kiley’s excellent article also features an explanation by Dr. Sam Zinner, a specialist in neurological development, of OCD’s medical origins.
“The human brain has a cluster of neurons called the basal ganglia. Put together, he explained, they’re the size of a walnut, and take in the deluge of cognitive, motor, memory, emotional and sensory information that floods through our brains when we, say, kick a soccer ball or watch out for poisonous snakes while walking through a swamp. The basal ganglia are supposed to filter out all the extraneous noise so we can focus on the task at hand. “In every picosecond of time,” Zinner said, “the basal ganglia have to decide what is relevant, what not to block out so you can survive.”
But the basal ganglia in brains with OCD — and related conditions, including Tourette syndrome and attention deficit hyperactivity disorder (ADHD) — are, in his words, “leaky filters.” Those leaks lead to information overload and behavior that, to the casual observer, might seem odd — like compulsively touching a magazine three times before picking it up, or hiding on a bathroom floor in costume during a ballet performance to avoid horrifying, intrusive thoughts.”
Hear Steve Loch describing his OCD symptoms in his own words and watch him dance in this captivating video by Seattle Times’ video editor Corinne Chin.

