The National Council on Disability calls for immediate action by the government to support the nation’s home and community-based services. Read more
healthcare
Mistreatment of physicians with disabilities is widespread, study finds
Journalist Jeffrey Bendix reports on a study that finds disabled physicians are often mistreated more than their fellow colleagues. Read more
Some doctors are reluctant to care for patients with disabilities, study finds
Journalist Jessica Bartlett reports on a study that found certain doctors don’t enjoy treating patients with disabilities because they find it more challenging. Read more
With Roe v. Wade Overturned, Disabled People Reflect on How It Will Impact Them
Disabled people are at high risk of being in a situation where they would need access to an abortion. Read the full story here.
‘Not Going Quietly’ – By Losing His Voice, Ady Barken Speaks for Others
The documentary ‘Not Going Quietly’ follows Ady Barken’s exploration of the disabled experience and documents the contribution of disabled activists fighting for universal healthcare. Read more here: https://womensenews.org/2021/09/not-going-quietly-by-losing-his-voice-he-speaks-for-others/
State Policies May Send People with Disabilities to the Back of the Line for Ventilators

By Liz Essley Whyte, Center for Public Integrity/The Daily Beast
An analysis by the Center for Public Integrity reveals that policies in at least 25 U.S. states have provisions that could de-prioritize health care for people with disabilities if cases of COVID-19 continue to ravage hospitals’ supplies.
Disability advocates have filed formal complaints in several states for their policies on who should get ventilators if hospitals run out. These policies take into account patients’ expected lifespan; need for resources, such as home oxygen; or specific diagnoses, such as dementia. Some policies even permit hospitals to take ventilators away from patients who use them as breathing aids in everyday life, and give the ventilators to other patients.
Twenty-five states have similar provisions in their rationing policies — and many other states either don’t have policies, or aren’t releasing them.
“There is a long history of people with disabilities being devalued by the medical system. That’s why we have civil rights laws,” said disability-rights activist Ari Ne’eman. “We don’t have an exception in our country’s civil rights laws for clinical judgment. We don’t take it on trust.”
Read the full article here: https://publicintegrity.org/health/coronavirus-and-inequality/state-policies-may-send-people-with-disabilities-to-the-back-of-the-line-for-ventilators/
5 Things Disabled People are Looking for in Healthcare Plans as the 2020 Elections Approach

By Andrew Pulrang, Rooted in Rights
A friend asks:
“Do you support Medicare For All? Why not? Don’t you believe everyone has a right to health care?”
Your coworker says:
“I think everyone should have healthcare, but how do we pay for it? And even if we can pay for it, how could we ever hope to pass such a huge and controversial plan?”
Meanwhile, your aunt wants to know:
“Do you really want the government in charge of your healthcare? And Is it fair that hardworking, responsible people should have to pay the medical bills for people who don’t even work? I don’t mean you of course …”
These are stereotypes, but nowadays they kind of ring true. They’re the sentiments that every disabled person even slightly engaged in the healthcare debate hears from every corner. That, and accusations of being a shill for “the other side” if you dare to ask critical questions and raise specific concerns as a disabled person. There’s no escape from it either, especially online. Now that 2020 campaigns are underway, you can’t plant a crutch or turn a wheelchair without running into someone’s passionate beliefs about healthcare. And they want you to believe, too. They’ll even point to your disability as a reason why you should support their position on healthcare.
The fact is that people with disabilities do have unique and important priorities that aren’t always addressed in healthcare plans. For people with disabilities, they matter more than ideology, poll-tested rhetoric, or political affiliations. This is the substance of the healthcare debate for the disability community.
Read the rest of Purlang’s article at https://rootedinrights.org/5-things-disabled-people-are-looking-for-in-healthcare-plans-as-the-2020-elections-approach/
Who bears the cost of Flagstaff’s minimum wage increase? Caregivers, for one.

For now, the impact of the state’s reimbursement law on the city’s finances is uncertain. Image: a photo of a piggy bank surrounded by loose coins. [Photo: Pixabay]
Click here to read this Cronkite News article online.
Mother asks Maricopa County prosecutors to release her daughter, a 19-year-old with mental illness, from Lower Buckeye Jail
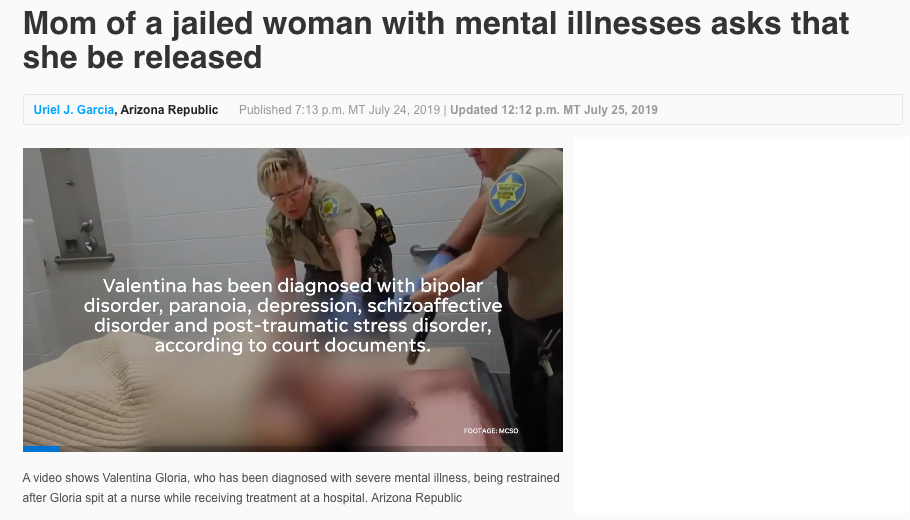
Valentina Gloria, a 19-year-old woman who has been diagnosed with several mental illnesses, has been detained at Maricopa County’s Lower Buckeye Jail for nearly six months, since February of this year. Now Vangelina Gloria, Valentina’s mother, is pleading for her teen daughter’s release.
Some say Valentina’s case exemplifies how our legal system criminalizes mental illness. Her predicament also highlights the ways in which our criminal justice system fails at providing quality mental healthcare to those who need it.
With support from Puente Arizona, a Phoenix-based migrant justice organization, Vangelina wrote a letter to Maricopa County Attorney Bill Montgomery earlier this week, requesting that he drop the charges against Valentina and release her from police custody. According to azcentral.com and court documents, Valentina has been diagnosed with bipolar disorder, paranoia, depression, schizoaffective disorder and post-traumatic stress disorder. Vangelina believes that being in jail is exacerbating her daughter’s mental health condition.
How did Valentina end up in jail?
In December 2018, [Valentina] Gloria was being treated in a behavioral health unit at St. Luke’s Hospital, where she was accused and arrested for spitting and punching two different nurses; she was then charged with two counts of aggravated assault. Then in May, a county judge ruled Valentina was incompetent to face the charges in court and ordered her to stay in jail to receive treatment through the County’s Restoration to Competency Program. A previous Arizona Republic analysis of Maricopa County’s Restoration to Competency Program expressed concerns about the program’s inefficiency and questioned the quality of the jailhouse mental healthcare provided by the county.
Click here to read an azcentral.com article recounting Vangelina’s efforts to secure Valentina’s release.
PHOENIX Magazine article by NCDJ board member Amy Silverman details lack of in-home care options
“Raising Phoenix: Home-Care Woes”

In addition to highlighting the need for better home-care services in the state, the Phoenix Magazine article also highlights Arizona’s failure to investigate the state’s Division of Developmental Disabilities, despite there being scores of formal complaints and well-documented concerns regarding the poor quality of the DDD’s in-home nursing services.
Click here to read Amy Silverman’s Phoenix Magazine article online.

